- Mon - Fri | 9:00AM - 9:00PMSat - Sun | 9:00AM - 5:00PM
Shoulder and Arm Conditions

Rotator Cuff injury
Rotator cuff syndrome is the most common shoulder injury. A relatively unstable shoulder joint is supported and movements executed by a small group of four muscles known as the rotator cuff which are responsible for shoulder rotation and form a cuff around the head of the shoulder bone.
Rotator cuff injuries vary from mild tendon inflammation (rotator cuff tendonitis), shoulder bursitis (inflamed bursa), calcific tendonitis (bone forming within the rotator cuff tendon) through to partial and full-thickness rotator cuff tears. Some may require surgery.
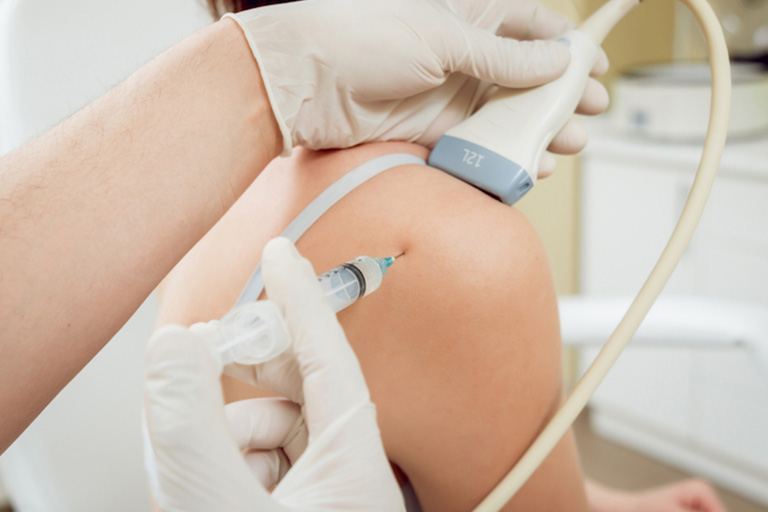
There are various types of rotator cuff injuries and hence a very experienced physiotherapist is very much necessary to diagnose the exact structures involved. A diagnostic ultrasound scan is a gold standard when it comes to identifying the specific rotator cuff pathology.
Common signs include clicking and painful arc while raising shoulder overhead, pain when lying on the affected shoulder that can extend from the top of your shoulder to your elbow. Muscle weakness and difficulty while reaching for your back.
Treatment does vary depending on the severity and the involved structure of rotator cuff injuries. You will be able to guided and managed by our shoulder experts to deliver the appropriate treatment and exercises for your rotator cuff injury.
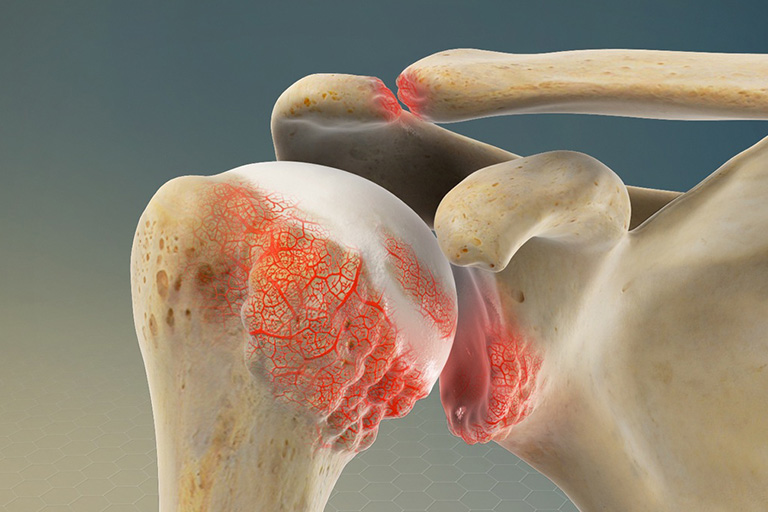
AC Joint Arthritis
The joint where the clavicle (collarbone) meets the scapula (shoulder blade) is called the Acromio- clavicular joint. Though not being a familiar joint but arthritis in the AC joint is actually more common than arthritis in the glenohumeral joint, the so-called shoulder joint commonly.
Diagnosing AC arthritis as the unique condition is important when it comes to treatment. Though shoulder arthritis occurs in the same region, the conditions are not one and the same. Patients with AC arthritis usually complain of pain associated with shoulder movements, but neck and arm pain may also be present which can complicate diagnosis.
Therefore, a careful and thorough clinical examination is the key part of making the diagnosis. Once diagnosed, our physiotherapists aim to provide a comprehensive rehabilitation to decrease muscle pain and spam with electrotherapy and soft tissue release initially followed by Strengthening and stretching exercises program to manage the condition.
Frozen Shoulder
Frozen shoulder or adhesive capsulitis as the name implies is a result of shoulder capsule inflammation and fibrous adhesions which gradually results in loss or reduction of your shoulder movement. Unfortunately, the reason why frozen shoulder starts is still being debated. In conditions such as diabetes, hyperthyroidism and hypothyroidism and incidentally after some shoulder surgeries the prevalence is greater.
After your initial session, a skilled physiotherapist should be able to make the right diagnosis and may help you avoid an arthrography or an MRI.
Frozen shoulder usually resolves well with physiotherapy and may require treatment for closer to 5 months and in some cases for about 24 months.
Most patients visit twice a month to learn the exercises and coping methods after the initial stages to manage pain and inflammation.
Shoulder Impingement
Impingement syndrome is when the soft tissues in and around the shoulder joint are repeatedly jammed up by the bones around them. Typically, this occurs when the arm is about halfway to the overhead position. Impingement syndrome can limit your ability to lift the arm at all, or to use it with any force in that position, such as hanging a cloth overhead or writing on a whiteboard.
Impingement syndrome usually involves inflammation of the supraspinatus tendon (supraspinatus tendinopathy or tendonitis), a part of the rotator cuff tendons, in people above 40 years old. In people under 40 years old, it usually involves inflammation of the subacromial bursa (subacromial bursitis). Narrowing of the space between the bony structures, a habitual round-shouldered or slumped posture resulting in poor functioning of the shoulder blade muscles, may most possibly predispose you to impingement. A sudden or recent change in activity with increase in the amount of overhead activities may also predispose you to an impingement problem.

Over the years, physiotherapy has been a very successful form of treatment for patients with impingement syndrome. A recent study in 2014 found that one year after a shoulder impingement injury, the patients who received physiotherapy had fewer episodes of shoulder impingement syndrome, requiring fewer visits to their GPs (37 per cent vs. 60 per cent) than the patients who had received initial corticosteroid injections. The patients who received injections often required additional injections for their impingement.
In the last decade, physiotherapy has become the first line of treatment for shoulder impingements. Of the various physiotherapy techniques, manipulation and low-level Laser seems to be the most effective form of treatment and hence we at river physio adhere to the successful treatment protocols as prescribed by the recent studies.
Shoulder Bursitis
Shoulder bursitis is an inflamed shoulder bursa. Your bursa is a fluid-filled sac that helps to reduce friction in your shoulder spaces. You have several bursae within your shoulder. Your subacromial bursa is the most commonly inflamed of the shoulder bursa.
Management of this condition will include laser and ultrasound therapy with prescribed exercises to strengthen your shoulder muscles whereby we reduce inflammation and offload the pressure over the involved bursa. Usually, the condition responds well to physiotherapy treatment.
Shoulder Arthritis
Shoulder Arthritis is the wear and tear damage to the articulating structures of your shoulder joints. The chances of you suffering shoulder arthritis are increased if your shoulder has been the active person involved in sports while young or injured the shoulder in the past. Researchers have confirmed that exercise is the best way of controlling arthritic pain, strengthening your muscles or keeping and improving your joint and muscle flexibility.
Regular Physiotherapy and exercise program will improve both your pain and range to move your shoulder better.
Your physiotherapist may use electrotherapy modalities such as LASER or TENS to improve your pain and subside inflammation.
Shoulder and arm injuries can affect your everyday lives. Come to River Physio Clinic in Singapore for friendly and professional care from expert physiotherapists. We treat over 2000 patients every month.
